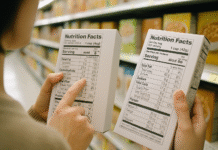
Hydration isn’t one-size-fits-all. “Everyday” hydration supports health and focus, while “sports” hydration adapts fluid and electrolyte intake to your sweat rate, intensity, duration, and environment to protect performance and safety. In simple terms: hit a sensible daily baseline, then layer sport-specific tactics on top. For quick orientation, here’s the gist: set a daily target (use urine color and thirst as checks), pre-hydrate before longer or hotter sessions, drink during exercise to roughly match sweat (without gaining weight), include sodium and carbs when efforts exceed ~60 minutes, and replace 125–150% of fluid losses afterward. These principles reflect current guidance from sports medicine groups and public health agencies as of August 2025.
Fast skim—how to apply this today
- Set a daily baseline (see Rule 1).
- 2–4 hours pre-workout: drink 5–10 mL/kg (add a small top-up if urine is still dark).
- During: target ~0.4–0.8 L/hour, guided by your sweat rate—never drink so much you gain weight.
- For efforts >60–90 min: use a drink with ~460–690 mg sodium/L and ~5–10% carbs.
- After: replace 1.25–1.5 L per kg of body mass lost, with sodium and food.
Medical note: If you have kidney, heart, or endocrine conditions—or take medications affecting fluid/electrolyte balance—ask a clinician for tailored advice. General tips below aren’t a substitute for medical care.
1. Set Your Everyday Baseline, Then Layer Sports Needs
Your daily baseline comes first: most adults do well aiming for roughly 6–8 cups of fluids across the day, adjusting for climate, activity, and diet; tea and coffee count, and pale-yellow urine is a practical sign you’re on track. Broaden that with intake from foods (fruit, vegetables, soups) and note that total water intake recommendations—3.7 L/day for men and 2.7 L/day for women—include both beverages and food moisture. These population-level numbers are averages, not minimums for every person; use thirst and urine color as everyday “feedback loops.” On training days, you’ll add sport-specific steps (Rules 2–5) on top of this baseline. In hot, humid weather—or at altitude—bump up fluids and electrolytes (see Rule 6).
1.1 Why it matters
- A consistent baseline keeps plasma volume stable, supporting blood pressure, temperature control, and cognition.
- Starting each workout already euhydrated reduces risk of early fatigue and heat illness.
- Separating “health” hydration from “performance” hydration helps you avoid both under- and over-drinking.
1.2 Mini-checklist
- Daily target: spread drinks from morning to evening; aim for pale-yellow urine.
- Count all fluids: water, milk, tea/coffee, sugar-free drinks; limit sugary beverages.
- Context cues: hotter days, high activity, illness, or breastfeeding → increase intake.
Synthesis: Nail the everyday basics first; then you’ll only need modest, strategic tweaks for training.
2. Pre-Hydrate on Training Days: 5–10 mL/kg, 2–4 Hours Out
For sessions in heat, durations >60–90 minutes, or key workouts, pre-hydrate so you start euhydrated with normal electrolytes. A practical target is 5–10 mL/kg of fluid 2–4 hours before exercise (that’s ~350–700 mL for a 70-kg person). If urine remains dark ~2 hours out, add another modest top-up (≈3–5 mL/kg). Flavor and cool temperatures can improve palatability; include a pinch of sodium via a lightly salted snack or a drink formulated with electrolytes if you’re a salty sweater or heading into heat. This timing allows absorption and a bathroom break before the session.
2.1 How to do it
- Calculate quickly: body mass (kg) × 5–10 mL = pre-exercise volume.
- Salty snack option: pretzels or broth if you’re prone to heavy salty sweat (white streaks on kit).
- Cool & sip: cooler fluids encourage drinking without GI slosh.
2.2 Numbers & guardrails
- Aim for euhydration + normal urine at start time; avoid overfilling.
- People sensitive to GI upset: favor steady sipping over chugging.
Synthesis: A timed, moderate preload sets you up to manage heat and prolong performance without gut discomfort.
3. Drink During Exercise to Match Sweat (0.4–0.8 L/h) Without Gaining Weight
During activity, the goal is to limit body mass loss to ≤2% while avoiding weight gain from over-drinking. A common workable range is ~0.4–0.8 L per hour, but your sweat rate—measured by weighing yourself before and after a representative session—should drive your plan. The sweat-rate formula: (pre-exercise mass − post-exercise mass) + fluid intake − urine output, divided by hours. Start with the range above, then refine with your data and conditions (pace, heat, humidity). Never exceed intake rates your gut tolerates; and don’t drink so much that your body mass increases, which raises hyponatremia risk. Lippincott Journals
3.1 Mini example
A 70-kg runner trains 90 minutes in warm weather, drinks 600 mL, and loses 1.1 kg:
- Mass loss = 1.1 kg → 1.1 L
- Sweat rate ≈ (1.1 L + 0.6 L) / 1.5 h = 1.13 L/h
- Next time, they might target ~0.8–1.0 L/h, split into sips every 10–15 minutes.
3.2 Common mistakes
- Copying others: sweat rates vary widely.
- Ignoring weight: if scale weight rises mid- or post-session, you over-drank.
- All water, long efforts: see Rule 4 for sodium and carbs.
Synthesis: Use your own sweat data to dial in intake; keep weight change within ~0–2% and you’ll protect performance and safety.
4. For Efforts >60–90 Minutes, Add Sodium (~460–690 mg/L) and Carbs (5–10%)
When duration and heat rise, electrolytes and carbohydrate help maintain plasma volume, support fluid absorption, and sustain pace. Sports medicine guidance supports drinks with ~20–30 mmol sodium/L (≈460–690 mg/L), ~2–5 mmol potassium/L (≈78–195 mg/L), and ~5–10% carbohydrate (glucose, sucrose, maltodextrin). Athletes with very high sweat sodium may need the higher end of sodium, or supplemental electrolytes, especially in hot environments and multi-hour events. For carbohydrates, many athletes perform well at 30–60 g/hour; advanced fueling can go higher with mixed carbohydrate sources, but gut tolerance varies. ResearchGate
4.1 How to choose a drink
- Label check: sodium per liter ~460–690 mg; carbs 5–10%.
- Taste test: pick flavors you’ll actually drink at pace.
- Mixing powders: measure by liter to hit targets reliably.
4.2 Guardrails
- Long, salty sweaters may need ~600–1,000 mg sodium/hour total (drink + foods), but introduce gradually and verify GI tolerance.
- Avoid super-concentrated mixes in heat without practice.
Synthesis: Past an hour, don’t rely on water alone—pair fluid with the right sodium and carbohydrate to keep pace steady and cramps at bay.
5. Recover Fast: Replace 125–150% of Fluid Lost, With Sodium and Food
After training or races—especially with back-to-back sessions—replace ~1.25–1.5 L per kg of body mass lost within a few hours, including sodium to aid retention. For example, if you finish 1 kg lighter, aim for ~1.25–1.5 L across the next 2–4 hours alongside a salty meal or electrolyte drink. Spreading intake improves comfort and absorption, and carbohydrate/protein in meals helps restore glycogen and repair muscle. In hot blocks, this “recovery window” is a performance multiplier for the next session.
5.1 Mini-checklist
- Weigh → plan: use post-exercise mass change to set your rehydration volume.
- Add sodium: soup, broth, salted eggs, pretzels, or an electrolyte drink.
- Don’t chug: pace your intake to limit bathroom losses.
Synthesis: Rehydrate to 125–150% of losses with sodium and food; you’ll feel better and be ready sooner.
6. Adjust for Heat, Humidity, Altitude, and Cold
Environment changes your needs. In heat and humidity, sweating rises and evaporation falls, so you’ll need higher fluid + sodium and more frequent cooling breaks. In everyday life during heatwaves, public health advice emphasizes regular water, shade, lighter clothing, and checking on vulnerable people. At altitude, increased breathing elevates fluid loss; appetite often drops, so plan fluids and salted foods proactively. Even in cold conditions, dry air and layers can sneakily dehydrate you—sip regularly. Athletes should schedule training during cooler hours, shorten intervals, and start conservatively in new environments.
6.1 Region notes (hot & humid climates)
- In monsoon-heat or tropical cities, sweat rates can exceed 1 L/h; adapt Rule 3 upward but never exceed hourly gut tolerance or gain weight.
- Plan shaded routes and chilled bottles; add sodium on long sessions.
6.2 Quick adaptations
- Heat: reduce intensity, extend recoveries, and pre-cool (ice slushie, cold towel).
- Altitude: prioritize fluids with electrolytes and carbohydrate; watch for AMS.
- Cold: warm fluids are fine; still monitor urine color.
Synthesis: Your plan is dynamic—environment dictates adjustments while core guardrails (Rule 3) stay constant.
7. Use Simple Monitoring: Body Mass, Urine Color, and Thirst
You don’t need a lab. Combine scale weight, urine color, and thirst to gauge hydration status. Daily: weigh at the same time and watch trends; pre/post-workout: track acute changes to estimate sweat rate and guide rehydration. For urine, the validated 8-color chart classifies pale yellow as well-hydrated and darker hues as hypohydrated (some foods/supplements can alter color—interpret in context). Thirst is an effective safety brake against over-drinking during steady efforts and cooler conditions; in prolonged heat or during intense racing, planned drinking based on your sweat data is often superior.
7.1 Mini-checklist
- Before & after: log body mass and fluids to refine your plan.
- Urine check: aim for 1–3 on the chart most of the day.
- Context matters: illness, vitamins, and beetroot can change urine color.
Synthesis: Triangulate weight, urine, and thirst—simple tools that keep your plan personalized and grounded. PMC
8. Choose the Right Fluids: Water, Sports Drinks, ORS, and Caffeine
Water works for everyday use and short sessions. For >60–90 minutes or heavy sweaters, sports drinks with measured sodium and carbohydrate improve fluid retention and energy delivery. When recovering from illness with diarrhea or vomiting, an oral rehydration solution (ORS)—glucose + electrolytes in specific ratios—enhances absorption and corrects deficits. Day to day, tea and coffee count toward hydration; moderate caffeine isn’t dehydrating in habitual consumers, but watch tolerance during long, hot events. For people with specific medical needs, discuss fluid choices with a clinician or dietitian.
8.1 Quick picks
- Everyday: water, milk, or sugar-free drinks.
- Long workouts: sports drink mixed to Rule 4 targets.
- GI illness: WHO-style ORS until symptoms settle.
Synthesis: Match the fluid to the job—most days water is enough; training days may call for sodium + carbs; illness calls for ORS. World Health Organization
9. Build Your Personal Hydration Plan: A Week-of-Training Template
Turn rules into routine. Start with your daily baseline and two sweat-rate tests (one cool, one hot). Slot pre-hydrate steps into days with long or intense sessions, and set during-exercise targets per session time and temperature. Pre-stage sodium/carbohydrate drinks for efforts >60–90 minutes. After sessions, check body mass change and recovery volume (125–150% of loss). Capture what worked and what didn’t; small adjustments (sip timing, flavor, sodium level) improve adherence and gut comfort. In heatwaves or altitude weeks, re-test sweat rate and adapt upward within gut limits.
9.1 Weekly mini-framework
- Mon–Fri: baseline fluids + short sessions → water; log urine color.
- Key days: T/Th long or intervals → pre-hydrate, drink to sweat rate with sodium/carbs, rehydrate 125–150%.
- Weekend long: practice fueling and sodium at race pace; weigh before/after.
- Review: adjust targets ±200–300 mL/h based on scale and comfort.
Synthesis: A written, repeatable plan—tested and tweaked—turns best-practice into better performance week after week.
FAQs
1) What’s the quickest way to tell if I’m hydrated on a normal day?
Aim for pale-yellow urine and steady energy; most adults do fine with ~6–8 cups of fluid spread through the day, more in heat or activity. Tea and coffee count; sugary drinks don’t help much nutritionally. Use thirst and urine color together for simple self-checks.
2) How do I measure my sweat rate without a lab?
Weigh before and after a typical session, track all fluids consumed, subtract any urine, and divide by hours: (pre − post + drinks − urine) / time. Do this in different weather to bracket your needs. Use the result to set your per-hour drinking target next time.
3) Is “drink to thirst” enough during workouts?
Often yes for short (<60–90 min), cool, or easy sessions. For long, hot, or high-intensity efforts, planned drinking based on your sweat rate better limits ≥2% body mass loss without risking over-drinking. Never drink so much that your weight increases.
4) How much should I drink during exercise?
A common starting range is 0.4–0.8 L/hour, then personalize using sweat-rate testing and gut comfort. Hotter, faster, and larger athletes usually sit higher; cooler or easier conditions trend lower.
5) What sodium/carbohydrate targets work best for long sessions?
Look for ~460–690 mg sodium per liter, ~5–10% carbohydrate, and ~78–195 mg potassium per liter. Many people perform well at 30–60 g carbs/hour; practice higher intakes gradually if racing longer. NSCA
6) How do I rehydrate after training or races?
Replace ~125–150% of your body mass loss across 2–4 hours. Include sodium (salty foods or electrolyte drink) to aid retention, and eat carbohydrate + protein for recovery.
7) What are the signs of drinking too much water?
Gaining weight during/after exercise, bloating, headaches, nausea, and confusion can signal exercise-associated hyponatremia—especially in events >4 hours with liberal fluid access. Prevention: don’t exceed sweat rate; include sodium on long efforts; heed thirst. Seek urgent medical care if severe symptoms occur.
8) Do I need sports drinks for everyday life?
No. For day-to-day hydration and short workouts, water (plus normal meals) is usually enough. Sports drinks are tools for longer/hotter sessions where you need sodium and carbohydrate.
9) How should I adapt for heatwaves or humid climates?
Train earlier/later, reduce intensity, increase fluids within gut limits, and add sodium for longer efforts. Public health guidance in heat also stresses shade, light clothing, and checking on vulnerable people.
10) Does illness change hydration strategy?
Yes. Fever, vomiting, and diarrhea raise fluid and electrolyte needs. Use oral rehydration solutions (glucose + electrolytes) to improve absorption until recovery, then return to your usual plan. Consult a clinician for persistent symptoms. NCBI
Conclusion
Optimal hydration blends two layers: a calm, consistent everyday baseline and a sports layer that adapts to your sweat rate, environment, and session plan. The baseline—regular fluids across the day, using urine color and thirst as guides—keeps you feeling sharp and resilient. The sports layer—timed pre-hydration, personalized during-exercise intake, and deliberate rehydration with sodium—protects pace, reduces perceived effort, and speeds recovery. Because needs vary, test your approach on training days, measure sweat rate in hot and cool conditions, and adjust in small steps. In heat or altitude, upshift thoughtfully; during illness, use ORS and rest. Keep notes, refine what works, and your plan will become effortless.
Ready to start? Pick one key session this week, run the weigh-in test, and set your first personalized per-hour target.
References
- American College of Sports Medicine Position Stand: Exercise and Fluid Replacement. ACSM / Medicine & Science in Sports & Exercise. 2007. PubMed
- Nutrition and Athletic Performance (Joint Position Statement). Academy of Nutrition & Dietetics, Dietitians of Canada, and ACSM. 2016. PubMed
- Dietary Reference Intakes for Water—Summary. National Academies (NASEM). 2004–2005. National Academies Press
- Heat and Athletes. U.S. CDC Heat Health. June 25, 2024. CDC
- Heat Stress: Hydration. NIOSH (CDC). 2017. CDC
- Statement of the Third International Exercise-Associated Hyponatremia Consensus Development Conference. Clinical Journal of Sport Medicine. 2015. British Journal of Sports Medicine
- Sweating Rate and Sweat Sodium Concentration in Athletes. Sports Medicine – Open. 2017. PMC
- Urinary Indices of Hydration Status. Armstrong et al., 1994. Int J Sport Nutr. PubMed
- Sweat Rate Calculation—Worksheet. CDC. 2008. CDC
- Water, Drinks and Hydration. NHS. Updated page (accessed 2025). nhs.uk
- Climate Change, Heat and Health—Fact Sheet. WHO. May 28, 2024. World Health Organization
- Planned Drinking Versus Drinking to Thirst. Kenefick, 2018. Sports Medicine. PubMed
- Compositional Aspects of Beverages Designed to Promote Hydration and Performance. Nutrients. 2023. PMC
- High-Altitude Travel and Altitude Illness (Yellow Book). U.S. CDC. Apr 23, 2025. CDC