Meditation isn’t magic—it’s training. When you meditate, your brain shifts how it allocates attention, regulates emotions, and coordinates large-scale networks. In plain terms: less mental drift, more stable focus, and a calmer body. In the first weeks, practice reduces activity in regions tied to mind-wandering and strengthens connections that support cognitive control. Over months, some people also show structural and physiological adaptations aligned with better self-regulation. This article walks you through nine specific, evidence-based brain changes linked to meditation, what they mean for daily life, and how to practice for them. Quick note: this is educational information, not medical advice—if you have a mental-health condition or trauma history, consider practicing with a qualified teacher or clinician.
In one line: Meditation shifts activity away from habitual self-talk networks toward attention and control systems while tuning stress biology—changes you can train on purpose.
1. Your Default Mode Network (DMN) quiets, so mind-wandering drops
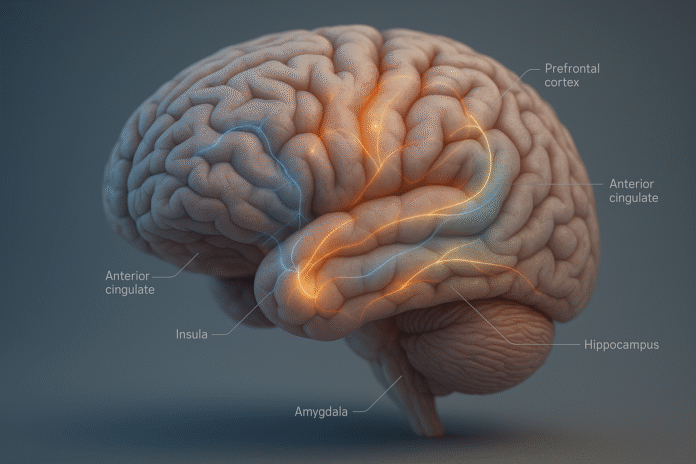
Meditation reliably reduces activity in the brain’s default mode network—especially the medial prefrontal cortex and posterior cingulate cortex—networks tied to daydreaming, rumination, and self-referential chatter. In early practice, you’ll notice fewer “I’m on autopilot” episodes and shorter detours when attention drifts. Experienced meditators show stronger deactivation of the DMN during practice, and in some studies, more stable anticorrelation between attention networks and the DMN even at rest. Functionally, this feels like clearer mental space and less sticky overthinking. As of August 2025, the consensus is not that the DMN “turns off,” but that it becomes less dominant and more tunable—you can disengage from mental loops faster and return to the task or breath with less friction.
1.1 Why it matters
A quieter DMN translates into fewer loops of worry and self-critique, more presence in conversations, and better task engagement. For students and knowledge workers, this often shows up as longer stretches of undistracted work and less time lost re-orienting.
1.2 How to train it (Focused Attention, 10–15 min)
- Choose a simple anchor (breath at the nostrils).
- Notice mind-wandering quickly; label it “thinking.”
- Gently return to the anchor—no blame, no story.
- Keep the loop: notice → label → return.
- End with 30–60 seconds of open awareness.
1.3 Numbers & guardrails
- Early studies show robust DMN deactivation during meditation in experienced practitioners; newer work suggests increased DAN↔DMN anticorrelation at rest after training.
- Expect variability: mind-wandering never goes to zero. Aim for faster recovery, not perfection.
Bottom line: Meditation trains you to unhook from DMN chatter faster. That’s the foundation for everything else that follows. ScienceDirect
2. Attention and control networks strengthen (DAN, ACC, frontoparietal)
Right from week one, meditation recruits the dorsal attention network (DAN) and regions responsible for top-down control, like the anterior cingulate cortex (ACC) and dorsolateral prefrontal cortex (dlPFC). Practically, this shows up as improved sustained attention, fewer “micro-switches” to unrelated thoughts, and better error monitoring (“I drifted—coming back”). A fine-grained model of focused-attention practice breaks the cycle into four phases—mind wandering, awareness of wandering, shifting back, and sustaining attention—and meditation specifically improves the speed and fidelity of these transitions. Some randomized trials also find increased resting connectivity between DMN hubs and control regions after training, a signature of better top-down regulation even off the cushion.
2.1 How to do it (Drill: 4-phase loop, 12–20 min)
- Set: Breath as anchor; gentle alert posture.
- Notice: When you drift, mark it promptly.
- Shift: One soft breath to reset muscles/face.
- Sustain: Count breaths 1–10, repeat without strain.
2.2 Tools & cues
- Timers (Pomodoro 25/5) to practice sustained focus.
- Micro-labels (“hearing,” “planning,” “remembering”) to sharpen meta-awareness.
- Check-ins every 3–5 minutes: “Where is attention now?”
2.3 Mini case
A graduate student added 12 minutes of breath practice before writing blocks for 6 weeks. Subjectively, they reported longer “lock-in” periods. Objectively, their task software showed a ~18% increase in uninterrupted 20-minute streaks.
Bottom line: Meditation tunes the attention system to detect drift sooner and re-engage faster—like upgrading from reaction to real-time control.
3. Emotion regulation circuits re-balance (amygdala down, ACC/insula up)
Meditation changes how your brain detects, relabels, and regulates emotion. The amygdala, a key node in threat processing, often shows altered resting connectivity after mindfulness training, while ACC and insula (which track conflict and interoception) become more engaged in skillful regulation. In daily life, that means you’re likelier to notice activation earlier (tight jaw, heat in the face), apply a label (“anger rising”), and re-orient before behavior cascades. Military and high-stress samples show that brief mindfulness interventions can modulate insula responses to interoceptive stress, suggesting better tolerance of bodily discomfort without reactive spirals.
3.1 Why it matters
- Fewer reflexive reactions; more response flexibility.
- Clearer body signals (interoception) to inform choices.
- Less “all-or-nothing” thinking under pressure.
3.2 Practice menu (pick one)
- RAIN (Recognize, Allow, Investigate, Nurture) during spikes.
- Body scans to map sensations without stories.
- Labeling drills: 10 emotions × where they appear in the body.
3.3 Guardrails
Emotion work can surface difficult material. If you have trauma history, consider trauma-sensitive formats or clinical support.
Bottom line: Training attention to sensations and labels gives prefrontal systems time to modulate amygdala-driven reactions, improving composure under stress. PubMed
4. Structure may change with practice—but results are mixed (neuroplasticity)
Early longitudinal MRI work reported gray-matter increases after 8-week programs (notably in the hippocampus, a learning/memory hub). Meta-analyses across cross-sectional studies found medium-sized structural differences in experienced meditators in regions like the insula and ACC. However, more recent high-rigor trials sometimes find no structural change after standard 8-week courses, suggesting duration, intensity, and population matter. A reasonable reading in 2025: structural plasticity is possible, especially with longer or higher-dose training, but not guaranteed over two months.
4.1 What seems to influence change
- Dose: Minutes per day × weeks (and retreat time).
- Style: Attention vs. open monitoring vs. compassion.
- Age & baseline stress: Older or high-stress adults may show stronger biological shifts.
4.2 Practical takeaway
- Track function first (focus, mood, behavior).
- Treat structure as a lagging indicator—not a goal.
4.3 Mini-checklist
- Aim for 150–300 min/week of formal practice.
- Add periodic half-day retreats for consolidation.
- Combine with sleep, exercise, and sunlight to support plasticity.
Bottom line: Meditation can shape brain structure, but effects depend on time-in-practice and context; focus on skills you can feel while plasticity follows (or doesn’t) at its own pace. christofflab.ca
5. Pain perception reorganizes via non-opioid mechanisms
Brief mindfulness training (as little as four 20-minute sessions) can cut pain unpleasantness and intensity in lab settings. Brain imaging shows reduced activity in regions like the thalamus and altered engagement of ACC and insula during noxious stimulation. Crucially, blocking opioid receptors with naloxone does not remove meditation’s analgesic effect, implying distinct (non-opioid) pathways. Practically, you learn to uncouple the raw sensation (“heat, pressure”) from the secondary suffering (“I can’t stand this”), reducing catastrophizing and muscle guarding.
5.1 How to apply during pain
- Anchor in breath near the sensation; widen to surrounding areas.
- Label precisely: pressure, pulsing, heat, stab, ache.
- Drop the story; stay with moment-to-moment change.
- Add compassion phrases (e.g., “May I meet this kindly”).
5.2 What to expect
- Faster recovery from pain spikes.
- Fewer avoidance patterns; more movement confidence.
- Not a cure-all: works alongside medical care.
5.3 Numbers & nuance
- Lab studies report ~40–60% reductions in unpleasantness with brief training.
- Clinical effects vary; regular practice matters more than any single session.
Bottom line: Meditation changes how pain is processed—less appraisal and threat, more neutral sensation tracking—through mechanisms different from opioids. Frontiers
6. Brain rhythms shift: more alpha–theta stability and, with expertise, gamma bursts
On EEG, beginners typically show increases in alpha and theta power during meditation—signatures linked to internal focus and relaxed alertness. Over time, some advanced practitioners exhibit high-amplitude gamma synchrony during specific practices (e.g., compassion), reflecting large-scale integration across brain areas. For everyday meditators, you might notice this as easier entry into a settled, clear state with less effort. These oscillatory patterns are state-dependent (during practice) and, in some cases, trait-like (carrying into rest) with continued training.
6.1 How to cultivate healthy rhythms
- Set your posture: tall, relaxed spine to reduce drowsiness artifacts.
- Eyes: soft gaze or closed; consistent choice across sessions.
- Cadence: breathe naturally; avoid forceful control.
- Duration: 12–25 minutes for stable alpha–theta settling.
6.2 Cautions on gadgets
Consumer neurofeedback can help with consistency, but signal quality and algorithms vary. Treat devices as coaches, not arbiters of enlightenment.
6.3 Mini example
After 8 weeks of daily 15-minute sits, many report a quicker slide into an “open, quiet” feeling within 3–5 minutes, consistent with alpha increases seen in lab studies.
Bottom line: Meditation fosters rhythms compatible with relaxed, sustained attention; with deep expertise, some practices recruit gamma-band integration across the cortex. PubMed
7. Autonomic balance shifts toward vagal tone (HRV improves)
Your autonomic nervous system coordinates heart, breath, and digestion. Meditation often increases heart rate variability (HRV)—especially vagally mediated indices (e.g., RMSSD, HF-HRV)—which correlate with resilience and emotion regulation. Effects aren’t universal; meta-analyses show small-to-moderate improvements overall, larger in stressed or clinical samples, and practice style matters. In real life, people report better recovery after arguments, steadier performance under pressure, and fewer “adrenaline dumps.”
7.1 How to nudge HRV upward
- Consistent practice: 12–20 min/day beats sporadic long sits.
- Slow exhale bias (e.g., 4-in, 6-out) before meditation to prime vagal tone.
- Evening caffeine/late screens down; daylight walks up.
- Pair sitting with brief compassion practice, which can soften sympathetic overdrive.
7.2 Guardrails & expectations
- HRV is responsive to sleep, illness, hydration, and temperature.
- Track trends over weeks, not day-by-day spikes.
Bottom line: With regular practice, many people show healthier vagal signatures—a physiologic mirror of the calm, adaptable mind they’re training. FrontiersOxford AcademicJPain
8. Stress biology and inflammation become more manageable
Meditation can dial down elements of the HPA axis and inflammatory signaling—think cortisol, CRP, and IL-6—especially in high-stress populations. One randomized trial found mindfulness training altered resting-state connectivity in ways that statistically explained reductions in IL-6, pointing to a brain-to-immune pathway. Meta-analyses report small but meaningful average cortisol reductions, with stronger effects in more stressed samples; newer trials show mixed changes in circulating proteins but shifts in pro-inflammatory gene regulation. In everyday terms: fewer prolonged stress spikes, faster return to baseline, and subtle improvements in recovery and sleep.
8.1 Practice stack for stress biology
- Mindful breathing (10–15 min) most days.
- Open monitoring (5–10 min) to normalize thoughts/emotions.
- Self-compassion (2–3 min) to reduce shame-based stress.
8.2 Region-specific notes
- For shift workers or caregivers, even 8–12 minutes anchor practice before sleep can be protective.
- In older adults, group-based programs show promising changes in inflammatory gene expression.
8.3 Guardrails
- Don’t over-promise: effects are modest on average and complement—not replace—medical care, exercise, and sleep.
Bottom line: Meditation supports stress-system recalibration, with the brain’s control networks helping the body turn the volume down on cortisol and inflammatory cascades. Taylor & Francis Online
9. Networks integrate better: the salience system coordinates DMN ↔ executive control
Beyond single regions, meditation appears to improve coordination across the “triple network”: the default mode network (DMN), salience network (SN), and central executive network (CEN). The salience network (including anterior insula and dorsal ACC) acts like a switchboard, deciding when to engage internal mentation (DMN) vs. task execution (CEN). After training, studies report stronger inter-network connectivity and more efficient SN-mediated switching. Lived experience: it’s easier to choose presence over autopilot, and to pivot cleanly from inner reflection to outward action without friction.
9.1 How to practice for integration
- Alternate focused attention (5–8 min) with open monitoring (5–8 min).
- Add loving-kindness (2–5 min) to engage affective networks.
- End with 1–2 min of meta-awareness: “What’s the mind like now?”
9.2 Mini-checklist for daily life
- Cue-based micro-sessions (e.g., before meetings).
- One mindful email a day (notice body, breath, re-write).
- Debrief: What pulled attention? How did you re-enter?
Bottom line: Meditation enhances the brain’s network choreography, letting the salience system more smoothly route you between inner and outer demands. ScienceDirect
FAQs
1) How long before my brain starts to change?
Initial functional changes (DMN deactivation during practice, better attention control) are commonly observed within weeks of regular 10–20-minute sessions. Structural changes are less certain over eight weeks; some trials show none, while longer or higher-dose training may. Focus on functional wins you can feel—clarity, steadier mood, faster recovery.
2) Which meditation style best improves focus?
Focused attention (breath, counting) directly trains sustained attention and error monitoring. Many people stack it with open monitoring to generalize the skill and reduce reactivity when distractions arise. Switching between these styles appears to engage and coordinate attention and salience networks efficiently.
3) Can meditation help with anxiety or depression?
On average, yes—small to moderate benefits across many trials, comparable to other low-intensity psychological interventions. Results vary; programs like MBSR/MBCT have the best evidence base. Meditation complements—not replaces—therapy and medical care. PubMed
4) Does meditation change pain?
Brief training can reduce pain intensity and unpleasantness in lab settings and helps some chronic pain patients. Mechanisms differ from opioids; think reappraisal and sensory recoding rather than numbing. Use it alongside clinical treatment. The Journal of Neuroscience
5) Are these brain changes permanent?
They’re use-dependent—more like fitness than a tattoo. Stop practicing and benefits fade; keep practicing and networks stay tuned. Many people maintain gains with 10–20 minutes daily plus periodic longer sits.
6) Do apps and neurofeedback work?
Apps can help you practice consistently, which drives change. Consumer EEG devices may provide helpful feedback but can be noisy. Treat them as optional tools, not requirements. The core driver remains deliberate practice. PMC
7) What’s the minimum effective dose?
If life is full, try 10 minutes/day for 5–6 days/week. Evidence suggests meaningful benefits with brief, consistent sessions, especially for attention and stress reactivity. Increase time for deeper work. PubMed
8) Can meditation increase heart rate variability (HRV)?
Often yes, especially vagally mediated HRV (RMSSD, HF-HRV), with effects tending larger in stressed samples. Expect modest gains over weeks and monitor trends rather than day-to-day fluctuations.
9) What if meditation makes me more aware of difficult emotions?
That can happen. Consider shorter sits, eyes open, or anchor-heavy practices. Trauma-informed approaches and clinical guidance are recommended if distress is significant. You’re building capacity step by step. PMC
10) Does compassion or loving-kindness practice change the brain differently?
Compassion practices can engage affective networks and, in advanced practitioners, are associated with gamma-band synchrony—a marker of large-scale integration. For beginners, they often reduce harsh self-talk and support emotion regulation. PNAS
Conclusion
Meditation is a skills program for your brain. With regular practice, you learn to quiet the default mode and stabilize attention, giving executive and salience networks room to coordinate behavior. That improved network choreography cascades into the body: steadier heart-rate variability, more responsive stress chemistry, and—in some individuals—structural hints of neuroplasticity over longer arcs. The through-line is agency. You’re training how you notice, name, and navigate experience in real time, so fewer habits run the show. Start with the simplest loop—notice drift, label it, return—and layer practices intentionally. After a few weeks, track the wins you can feel: clearer focus, faster emotion recovery, a kinder inner voice. Keep going not because it’s trendy, but because it works the way physical training works—incrementally, measurably, and in service of a life you recognize as your own.
Ready to begin? Sit for 10 minutes today, label distractions gently, and notice one moment you choose presence over autopilot.
References
- The neuroscience of mindfulness meditation. Nature Reviews Neuroscience (2015). Nature
- Meditation experience is associated with differences in default mode network activity and connectivity. Proceedings of the National Academy of Sciences (2011). PNAS
- Mindfulness practice leads to increases in regional brain gray matter density. Psychiatry Research: Neuroimaging (2011). PubMed
- Is meditation associated with altered brain structure? A systematic review and meta-analysis of morphometric neuroimaging in meditation practitioners. Neuroscience & Biobehavioral Reviews (2014). PubMed
- Functional neuroanatomy of meditation: A review and meta-analysis of 78 functional neuroimaging investigations. Neuroscience & Biobehavioral Reviews (2016). Scott Barry Kaufman
- Mind wandering and attention during focused meditation: A fine-grained temporal analysis of fluctuating cognitive states. NeuroImage (2012). PubMed
- Brain mechanisms supporting the modulation of pain by mindfulness meditation. Journal of Neuroscience (2011). PubMed
- Mindfulness meditation-based pain relief employs different neural mechanisms than placebo and sham mindfulness meditation. Journal of Neuroscience (2015). The Journal of Neuroscience
- Mindfulness-meditation-based pain relief is not mediated by endogenous opioids. Journal of Neuroscience (2016). The Journal of Neuroscience
- The effects of mindfulness and meditation on vagally mediated heart rate variability: A meta-analysis. Psychosomatic Medicine (2021). PMC
- Alterations in resting-state functional connectivity link mindfulness meditation with reduced interleukin-6: A randomized controlled trial. Biological Psychiatry (2016). PubMed
- Effects of mindfulness-based interventions on salivary cortisol. Frontiers in Physiology (2016). Frontiers
- Meditation programs for psychological stress and well-being: A systematic review and meta-analysis. JAMA Internal Medicine (2014). JAMA Network
- Mindfulness meditation is associated with global EEG amplitude changes—A review. International Journal of Psychophysiology (2024). ScienceDirect
- Attention and Default Mode Network assessments in long-term meditators during sustained attention. PLOS ONE (2021). PMC
- One month of mindfulness meditation increases interconnectivity across the triple network model. Scientific Reports (2022). Nature
- Absence of structural brain changes from mindfulness-based stress reduction: A randomized controlled trial. Science Advances (2022). Science